How to Build Patient Management Software? Processess, Features, Costs
Modern healthcare is undergoing a major digital shift. Hospitals, clinics, and diagnostic centers are increasingly relying on healthcare software solutions that streamline patient data handling, reduce paperwork, eliminate manual errors, and improve communication across departments. Patient management software plays a crucial role in this transformation by centralizing essential clinical and administrative operations—covering everything from registration and appointments to billing and follow-ups.
As healthcare demand grows and patient expectations evolve, such systems help providers deliver faster, safer, and more efficient care.
- Market Demand and Digital Transformation in Healthcare
- What Is Patient Management Software?
- Why Hospitals, Clinics, and Telemedicine Providers Use Patient Management Software?
- How It Differs from an EHR/EMR and When to Use Which
- Key Features of Patient Management Software
- Patient Registration and Onboarding
- Digital Health Records Management
- Appointment Scheduling and Calendar Automation
- Medical Billing and Insurance Processing
- E-Prescriptions
- Telemedicine and Virtual Consultations
- Patient Portal and Mobile App Access
- Lab Integration and Test Reports
- Alerts, Notifications, and Reminders
- Role-Based Access & Security Features
- Analytics and Performance Dashboards
- Step-by-Step Process to Build Patient Management Software
- Requirement Analysis and Workflow Mapping
- Competitor and Market Research
- UI/UX Design and Wireframing
- Choosing the Technology Stack
- Backend, Frontend, and Mobile App Development
- Integration with EHR/EMR Systems
- Data Security, Compliance, and Encryption
- QA Testing and Performance Validation
- Deployment and Cloud Setup
- Maintenance, Support, and Upgrades
- Technology Stack for Patient Management Software
- Cost of Developing Patient Management Software
- Patient Registration and Onboarding
- Digital Health Records Management
- Appointment Scheduling System
- Billing and Insurance Processing
- E-Prescription Module
- Telemedicine and Virtual Consultations
- Patient Portal and Mobile App
- Lab Integration and Test Reports
- Alerts, Notifications, and Reminders
- Analytics and Performance Dashboards
- Security and Role-Based Access
- Future Trends in Patient Management Software
- 1) Artificial Intelligence and Machine Learning
- 2) Predictive Analytics and Data-Driven Insights
- 3) Telemedicine and Remote Patient Monitoring
- 4) Cloud Computing and Scalability
- 5) Mobile Health (mHealth) and Patient Engagement
- 6) Integration with Wearables and IoT Devices
- 7) Automation of Administrative Workflows
- 8) Enhanced Security and Compliance
- 9) Interoperability and Standardized Data Exchange
- 10) Artificial Intelligence-Powered Chatbots and Virtual Assistants
- Sum up
- FAQs
- What is patient management software development, and why is it important?
- What are the key features included in patient management software development?
- How does patient management software development differ from hospital management software development?
- What factors influence the cost of patient management software development?
- How is patient management software improving patient care and operational efficiency?
Market Demand and Digital Transformation in Healthcare
The global healthcare industry is rapidly integrating digital tools to enhance operational outcomes. Rising patient volumes, increased adoption of telemedicine, and the urgent need for interoperable digital records have made patient management systems a necessity rather than a choice. Healthcare organizations now seek solutions that improve patient experience, optimize staff productivity, and ensure data accuracy across all processes.
This growing demand has encouraged both startups and enterprises to invest in scalable, secure, and intuitive patient management platforms that can handle everything from basic administrative duties to complex clinical workflows.
Looking for? Best Healthcare Agentic AI Developers
What Is Patient Management Software?
Patient management software is a centralized digital system designed to handle the administrative and clinical lifecycle of a patient within a healthcare facility. At its heart, it replaces fragmented paper processes and isolated spreadsheets with a single source of truth — a secure database where patient demographics, visit histories, diagnoses, medications, billing records, lab results, and communications live together.
The primary goals are to reduce manual work, eliminate duplicate data entry, minimize errors, accelerate patient flow, and provide clinicians and administrators with the information they need when they need it. When designed well, it becomes the operational backbone of a clinic, hospital wing, or multi-site health network.
This software is not just a digital filing cabinet. It actively orchestrates workflows: registering patients, verifying insurance, assigning rooms, scheduling follow-ups, generating invoices, and feeding data to clinical decision-support modules.
We can say, patient management software bridges front-desk efficiency with clinical continuity. The process of patient management software development must therefore combine domain knowledge (clinical and administrative workflows) with strong software engineering, data security, and user-centered design.
Read once! Agentic Healthcare Is Transforming Patient Experience
Why Hospitals, Clinics, and Telemedicine Providers Use Patient Management Software?
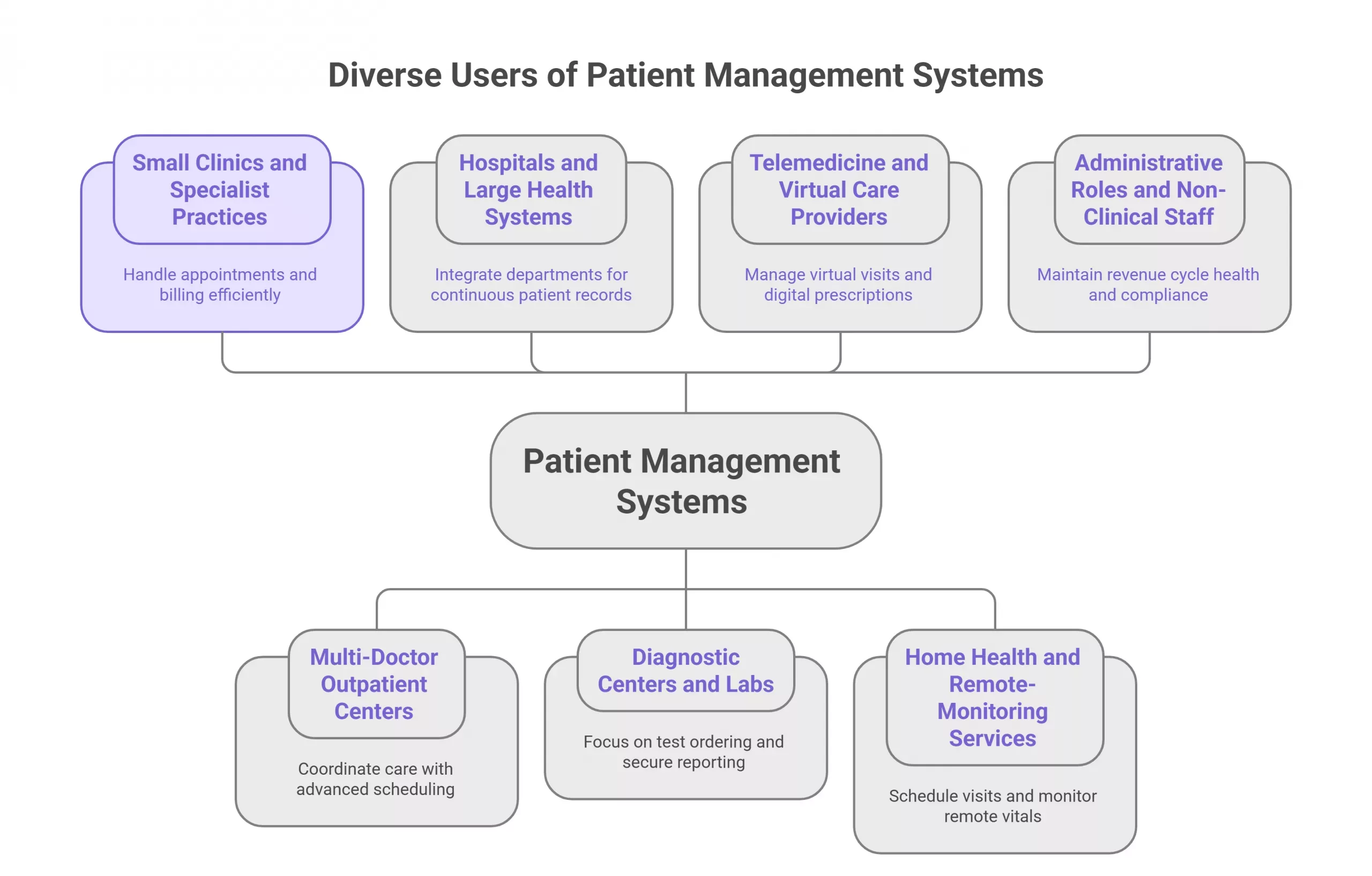
Patient management systems serve a broad spectrum of healthcare providers and stakeholders. Typical users include:
- Small clinics and specialist practices: These organizations use patient management software to handle appointments, maintain simple electronic records, and automate billing, allowing a lean staff to manage a steady patient load without administrative bottlenecks.
- Multi-doctor outpatient centers and group practices: These require more advanced scheduling, role-based access, and shared patient histories so multiple clinicians can coordinate care.
- Hospitals and large health systems: Larger facilities need solutions that integrate across departments — emergency, inpatient wards, surgery, radiology, labs, and billing — to maintain a continuous patient record through complex care journeys. In many cases, hospitals will combine a patient management system with enterprise systems; sometimes this is called hospital management software development when the scope expands to facility-wide operations.
- Diagnostic centers and labs: These organizations focus on test ordering, result reporting, and secure delivery of lab reports to referring clinicians and patients. Integration with laboratory information systems (LIS) is a common requirement.
- Telemedicine and virtual care providers: With virtual visits, patient intake, identity verification, video conferencing, and digital prescribing all become components of the patient management workflow. Telemedicine providers rely on the system to reconcile virtual visit data with the patient’s longitudinal record.
- Home health and remote-monitoring services: These use patient management tools to schedule home visits, capture remote vitals, and trigger alerts when thresholds are breached.
- Administrative roles and non-clinical staff: Front-desk clerks, billers, coding specialists, and practice managers interact heavily with the administrative side of the system to maintain revenue cycle health and compliance.
How It Differs from an EHR/EMR and When to Use Which
Many people conflate patient management software with EHR (Electronic Health Record) or EMR (Electronic Medical Record) systems. While they share some overlapping functions, there are clear distinctions worth noting, especially when evaluating solutions from EHR software development companies. These companies often build advanced systems focused on clinical documentation, detailed medical histories, and regulatory compliance, whereas patient management software typically centers on scheduling, communication, and workflow efficiency.
- Patient management software emphasizes operational workflows: registration, scheduling, billing, appointment reminders, and patient communication. Its main focus is keeping the practice running smoothly and ensuring the administrative lifecycle is efficient.
- EHR/EMR systems prioritize clinical documentation, charting, problem lists, medication reconciliation, and clinical decision support. They are focused on the clinical record and standards for clinical data exchange.
- When both are needed: Most modern implementations blend both capabilities — administrative functionality from patient management systems plus clinical depth from EHR/EMR modules. In a small clinic, a single system may serve both roles; in a large hospital, specialized EHR modules may be integrated with a separate patient management solution. Deciding which to prioritize depends on clinical complexity, regulatory needs, interoperability requirements, and budget.
Business Value and ROI
Investing in patient management software offers measurable returns when implemented thoughtfully. Time savings at registration and billing reduce front-desk staffing pressure.
- Automated appointment reminders lower no-show rates, increasing billable visits. Faster access to patient histories reduces duplicate tests and improves throughput.
- On the revenue side, better coding and claims management speed up reimbursements and reduce denials.
- On the clinical side, easier access to records improves care coordination and can reduce medical errors.
When you calculate ROI, include reduced administrative FTEs, lower paper and storage costs, fewer billing denials, higher patient throughput, and—crucially—improved patient satisfaction, which drives retention and referrals.
Key Features of Patient Management Software
Patient Registration and Onboarding
A foundational feature of any patient management system is digital registration. Instead of manually filling in paper forms at the front desk, patients can submit demographic details, medical history, and insurance information through a tablet, kiosk, or mobile app.
Automated onboarding ensures the data is accurate, instantly validated, and securely stored. This reduces wait times and administrative workload while improving the overall onboarding experience. Features often include ID scanning, insurance verification, document uploads, consent form signing, and profile creation that syncs across all departments.
Digital Health Records Management
Digital health record management allows healthcare providers to maintain detailed logs of a patient’s medical conditions, visit history, prescriptions, allergies, treatment plans, lab reports, and physician notes.
Instead of searching through physical files, clinicians and staff have immediate access to all relevant information. The system typically includes quick search filters, real-time updates, and structured data fields that prevent errors and inconsistencies. This module is essential for improving clinical decision-making and ensuring continuity of care throughout the patient’s medical journey.
Appointment Scheduling and Calendar Automation
Scheduling is a critical operational component, especially for busy clinics and hospitals. The software provides an intelligent calendar that syncs across departments and practitioners. Patients can book appointments online, reducing phone traffic and administrative burden.
Automated reminders significantly reduce no-shows, while color-coded calendars help staff visualize daily workloads. Some systems include smart scheduling algorithms that prioritize urgent cases, balance physician availability, and detect appointment conflicts before they occur.
Medical Billing and Insurance Processing
Billing is often one of the most challenging aspects of healthcare operations. Patient management software simplifies this with automated invoice generation, coding support, claim submission, payment tracking, and integration with insurers.
The system ensures that each service item is captured accurately, minimizing claim denials and accelerating reimbursements. Automated billing workflows reduce errors and ensure compliance with local medical billing regulations. This feature is indispensable for ensuring timely revenue cycle management.
E-Prescriptions
E-prescription functionality helps clinicians digitally prescribe medications and send them directly to pharmacies. This eliminates handwritten errors and ensures proper dosage, drug interaction checks, and prescription history tracking.
Patients receive their prescriptions through email or the patient portal, making it easy to refill medications or share them with pharmacies. Digital prescribing also improves safety by enabling real-time alerts for potential drug interactions or allergies.
Telemedicine and Virtual Consultations
In modern healthcare, virtual care has become a necessity rather than a luxury. Telemedicine features allow patients to meet doctors online via video calls, chat, or voice. The software integrates secure video conferencing tools, patient identity verification, online payments, digital visit summaries, and virtual care documentation. This module extends a healthcare provider’s reach, enabling remote consultations, follow-ups, and chronic condition management—especially valuable in rural or underserved areas.
Patient Portal and Mobile App Access
A patient portal empowers patients to play an active role in their healthcare. Through web or mobile apps, patients can book appointments, download reports, communicate with doctors, update personal data, request refills, and track treatment plans.
This transparency builds trust and enhances patient engagement. The portal also improves administrative efficiency by reducing incoming calls for routine tasks.
Lab Integration and Test Reports
Diagnostics and laboratory tests are central to most patient workflows. Patient management software supports seamless integration with laboratories, enabling electronic test ordering and automatic importing of results into the patient’s record. This eliminates delays, reduces errors, and ensures that both patients and clinicians have immediate access to lab results. Advanced systems offer structured lab report formats, comparison charts, and alerts when results fall outside normal ranges.
Alerts, Notifications, and Reminders
Notifications ensure that all stakeholders—patients, doctors, and administrators—stay updated. The system can send reminders for appointments, medication schedules, report availability, billing dues, and upcoming preventive screenings. This automation increases patient compliance, reduces no-shows, and keeps operations running smoothly. Internally, staff may receive alerts about critical lab values, pending tasks, or workflow bottlenecks.
Role-Based Access & Security Features
Security is crucial in healthcare software. Role-based access control allows administrators to define who can access which data. Doctors, nurses, lab technicians, billing clerks, and administrators each get tailored permissions that align with their responsibilities. This prevents unauthorized access and reduces the risk of data breaches. The system typically includes audit logs, multi-factor authentication, encrypted storage, and secure communication protocols to protect sensitive patient data.
Analytics and Performance Dashboards
To optimize healthcare operations, decision-makers need data insights. Built-in dashboards display key metrics such as patient flow, appointment utilization, revenue cycles, clinical performance indicators, and patient satisfaction scores.
These analytics help in identifying bottlenecks, improving operational efficiency, forecasting trends, and making data-driven decisions. Advanced analytics modules may also include predictive models for patient risk assessment, helping providers act proactively.
Step-by-Step Process to Build Patient Management Software
Requirement Analysis and Workflow Mapping
The first and most decisive step in building patient management software is understanding the healthcare organization’s workflows, needs, and objectives. Healthcare environments differ widely — a cardiology clinic, a multi-specialty hospital, a telemedicine startup, and a diagnostic center each have distinct processes.
During requirement analysis, the development team meets with administrators, physicians, nurses, lab staff, and billing personnel to document every workflow. This includes patient intake, triage processes, consultation flow, lab coordination, billing cycles, discharge procedures, and follow-up mechanisms.
Many Telehealth Software Development Firms also follow this structured approach because understanding clinical workflows early ensures that the final system supports both in-person and remote care processes.
Mapping these processes visually using workflow diagrams helps clarify system behavior and prevents misunderstandings.
Additionally, the development team identifies pain points such as long wait times, manual paperwork, appointment congestion, billing inaccuracies, or poor record accessibility. These insights shape the feature set, integrations, automation rules, and security standards.
During this phase, compliance requirements and data privacy standards are also defined so they can be embedded from the very beginning of the patient management software development lifecycle.
Competitor and Market Research
To build a successful and competitive system, the team must analyze existing patient management solutions in the market. This includes studying their features, UI patterns, pricing models, strengths, and weaknesses.
Competitor research helps identify gaps that can become opportunities—for example, telemedicine integration, intuitive mobile interfaces, advanced analytics, or faster onboarding processes.
Market research also includes analyzing regional healthcare regulations, insurance demands, patient expectations, and technology trends.
Understanding these dynamics ensures that the software not only meets clinical and administrative needs but also aligns with market demand. This step reduces risk by helping the development team create a product that stands out in usability, efficiency, and compliance.
UI/UX Design and Wireframing
Design is critical in healthcare software because users such as nurses, physicians, and administrators operate under high pressure. A poorly designed system can slow down workflows or increase error rates. During this stage, designers create wireframes and prototypes that illustrate how each screen will function.
The UI/UX strategy focuses on:
- Intuitive navigation for fast task completion
- Clear visual hierarchy for clinical information
- Minimalist layouts to prevent cognitive overload
- Accessibility features for diverse user groups
- Mobile-responsive design for tablets and smartphones
Interactive prototypes are often tested with real users—front-desk staff, doctors, and technicians—to gather feedback and refine the interface before coding begins. This ensures the final design directly supports real-world healthcare tasks.
Choosing the Technology Stack
Selecting the right technology stack shapes the performance, scalability, and security of the software. The stack includes frontend frameworks, backend languages, mobile app platforms, databases, and infrastructure tools.
Common choices include:
- Frontend: React, Angular, Vue.js
- Backend: Node.js, Python (Django/Flask), Java, .NET
- Mobile: Flutter, React Native, Swift, Kotlin
- Database: PostgreSQL, MySQL, MongoDB
- Cloud: AWS, Azure, Google Cloud
- Integrations: Twilio (SMS), Stripe/PayPal (payments), insurance APIs, HL7/FHIR interfaces
The choice depends on scalability needs, integration complexity, and regulatory requirements. A well-chosen stack ensures the system can support large patient volumes, fast data retrieval, and smooth integrations.
Backend, Frontend, and Mobile App Development
Once the design and tech stack are finalized, development begins.
Backend development focuses on building the core logic: user management, patient data structures, appointment logic, billing workflows, and security frameworks. It also handles API development for third-party integrations.
Frontend development brings the UI/UX design to life. Developers build user interfaces for dashboards, patient profiles, scheduling calendars, billing screens, and report views. The focus is on speed, clarity, and usability.
Mobile app development is essential today, as patients prefer accessing services on smartphones. The mobile component includes appointment booking, telemedicine access, medical record downloads, and notification management. Developers ensure all data syncs in real time across devices.
Throughout development, modular architecture ensures scalability, maintainability, and integration readiness.
Integration with EHR/EMR Systems
Most healthcare solutions providers already use certain software tools such as EHR, EMR, LIMS, or RIS. Patient management software must seamlessly integrate with these systems to maintain unified patient records.
Standard healthcare data formats such as HL7 and FHIR are used to enable interoperability between systems.
Integrations may include:
- Laboratory systems (LIS)
- Radiology systems (RIS)
- Pharmacy systems
- Insurance and billing networks
- Telemedicine platforms
These integrations ensure that patient test results, scans, prescriptions, and billing codes flow effortlessly between departments. Smooth interoperability reduces redundancy, enhances safety, and accelerates clinical workflows.
Data Security, Compliance, and Encryption
Security is a non-negotiable element of healthcare software. Sensitive patient data must be protected at all levels: storage, transmission, and access.
Security measures typically involve:
- End-to-end encryption
- Role-based access control
- Multi-factor authentication
- Secure APIs
- Audit trails
- Regular penetration testing
Compliance with regulations is also mandatory. Depending on the region, this may include HIPAA, GDPR, or local healthcare standards. Compliance requirements influence how data is stored, accessed, transmitted, and backed up. At this stage, developers implement compliance-specific safeguards that ensure the system cannot be exploited or misconfigured.
QA Testing and Performance Validation
Quality Assurance (QA) is critical because healthcare workflows cannot tolerate errors. Testing covers multiple categories:
- Functional testing to ensure each feature works as designed
- Usability testing to confirm intuitive workflows
- Integration testing to verify data flows across systems
- Security testing for vulnerabilities and breaches
- Load and performance testing to ensure the system handles peak patient volumes
Testers also simulate real-world scenarios such as appointment overload, billing conflicts, lab report delays, and data entry errors. Only after each module passes these extensive checks does the software move toward deployment.
Looking for? AI-Powered Software Testing Tools
Deployment and Cloud Setup
After testing, the software is deployed on cloud servers or on-premise systems, depending on the healthcare provider’s requirements. Cloud deployment is increasingly preferred due to its scalability, reduced maintenance costs, and built-in security features. The deployment process includes configuration of environments, domain setup, load balancing, security hardening, and data migration from legacy systems.
User onboarding and staff training run parallel to initial deployment. Transitioning staff from manual systems or older software requires clear instructions, demo sessions, and continuous support.
Maintenance, Support, and Upgrades
Even after launch, the patient management system requires ongoing maintenance. This includes fixing bugs, upgrading the UI, improving performance, and adding new modules. Healthcare regulations frequently evolve, so compliance updates must be implemented periodically. As patient volume grows, the infrastructure may need scaling.
Maintenance also involves monitoring uptime, optimizing servers, updating integrations, and providing customer support. Continuous improvement ensures the software remains relevant, secure, and aligned with clinical and administrative objectives.
Technology Stack for Patient Management Software
| Category | Technologies / Tools | Purpose & Detailed Explanation |
|---|---|---|
| Frontend Technologies | React, Angular, Vue.js | These frameworks help create fast, interactive, and user-friendly interfaces. React is ideal for scalable UI, Angular suits enterprise-level structure, and Vue.js offers flexibility and simplicity. They ensure smooth navigation, responsive dashboards, and quick access to patient data. |
| Backend Technologies | Node.js, Python (Django/Flask), Java, .NET | Backend technologies handle core logic, authentication, patient records management, billing workflows, scheduling algorithms, and API endpoints. Node.js supports real-time features, Python offers rapid development and strong libraries, Java and .NET are preferred for large enterprise-grade hospital systems due to security and robustness. |
| Mobile App Development | Flutter, React Native, Swift, Kotlin | Flutter and React Native enable cross-platform apps with a single codebase. Swift (iOS) and Kotlin (Android) offer high performance for native apps. These technologies power patient portals, telemedicine modules, notifications, and appointment management on mobile devices. |
| Databases | PostgreSQL, MySQL, MongoDB, Redis | SQL databases like PostgreSQL/MySQL manage structured health records, billing data, and scheduling. MongoDB handles flexible unstructured clinical notes or prescription logs. Redis is used for caching to speed up performance in high-volume healthcare environments. |
| Cloud Platforms | AWS, Microsoft Azure, Google Cloud | Cloud platforms provide scalable infrastructure, automated backups, high availability, and built-in compliance tools. AWS is popular for large-scale deployments, Azure integrates well with enterprise systems, and Google Cloud offers strong analytics capabilities. |
| API Integrations | Twilio (SMS/OTP), Stripe/PayPal (Payments), HL7, FHIR APIs | Integrations allow smooth communication between systems. Twilio handles appointment reminders, OTPs, and alerts. Stripe/PayPal support online payments. HL7 and FHIR APIs ensure interoperability with other healthcare platforms (EHR/EMR, labs, radiology). |
| Security & Compliance Tools | JWT, OAuth2.0, SSL/TLS Encryption, IAM Tools, Firewalls | Ensures secure authentication, encrypted data transfer, protected access controls, and compliance with healthcare privacy standards. These are vital for safeguarding patient records and preventing breaches. |
| DevOps & Deployment Tools | Docker, Kubernetes, Jenkins, GitHub Actions | Ensure smooth development, continuous integration, automated deployment, and scalable operations. Kubernetes helps run patient management software reliably under heavy workloads. |
| Analytics & Reporting Tools | Power BI, Tableau, Elastic Stack | These tools enable the software to offer dashboards, clinical insights, visual reports, patient flow analysis, revenue forecasting, and operational performance metrics. |
Cost of Developing Patient Management Software
Developing patient management software requires careful planning and budgeting, as costs vary depending on features, integrations, compliance requirements, and system complexity. Below is a detailed breakdown of the main cost components in a paragraph-style format with clear subheadings.
Patient Registration and Onboarding
The patient registration and onboarding module is the foundation of any patient management system. It includes digital forms, identity verification, insurance information capture, document uploads, and profile creation. The goal is to streamline front-desk operations and reduce manual paperwork.
Developing this module requires designing an intuitive user interface, backend support for secure data storage, and integration with other modules like scheduling and billing. For a typical system, this module costs between $4,000 and $8,000, depending on the complexity of validation, automation, and user interface design.
Digital Health Records Management
Digital health records management allows storage and retrieval of patient medical histories, diagnoses, prescriptions, allergies, treatment plans, and visit notes. This module is crucial for clinicians and administrators to access comprehensive patient information quickly. It requires a robust backend, secure data structures, and features like search, sorting, and reporting.
A well-structured health records module ensures continuity of care and reduces errors. Developing this module generally costs $10,000 to $25,000, based on the level of functionality and integration with other modules.
Appointment Scheduling System
Scheduling appointments efficiently is critical in reducing no-shows and optimizing staff workload. A modern scheduling system includes doctor calendars, real-time availability, conflict detection, automated reminders, and patient self-booking capabilities.
The development of this module requires integrating real-time updates, notifications, and calendar synchronization features. A complete appointment scheduling module typically costs between $8,000 and $18,000, depending on automation, complexity, and multi-doctor management features.
Billing and Insurance Processing
Billing and insurance processing are among the most critical and complex modules. This includes automated invoice generation, insurance claim submission, payment tracking, and error detection. Integration with insurance providers and support for coding standards ensures accuracy and faster reimbursement.
Developing a billing and insurance module involves both frontend and backend complexity and typically costs $12,000 to $30,000, depending on the number of supported services and integration depth.
E-Prescription Module
E-prescription functionality allows clinicians to create digital prescriptions, check drug interactions, and send prescriptions directly to pharmacies. This module increases patient safety, reduces errors, and speeds up pharmacy workflows.
Integrating drug databases, interaction checks, and secure delivery mechanisms increases development complexity. The cost for this module generally ranges from $6,000 to $12,000.
Telemedicine and Virtual Consultations
With the rise of remote healthcare, telemedicine modules are essential for modern patient management systems. This includes secure video consultations, chat functionality, appointment logs, digital visit summaries, and billing integration.
Developing this module requires real-time communication capabilities, strong security measures, and compliance with healthcare regulations. Telemedicine functionality typically costs $15,000 to $40,000, depending on the level of integration and real-time features.
Patient Portal and Mobile App
Patient portals and mobile applications enhance patient engagement by allowing users to book appointments, access medical records, receive notifications, and communicate with providers. Developing a mobile-friendly portal requires both frontend and backend development, user authentication, data synchronization, and push notification support.
This is often one of the more expensive modules, with costs ranging from $20,000 to $50,000, depending on platform support (iOS, Android, web) and feature complexity.
Lab Integration and Test Reports
Integrating laboratory systems allows automated test ordering, electronic result retrieval, and structured reporting within the patient record. This module reduces delays, eliminates manual entry errors, and provides timely information to both patients and clinicians. Depending on the number of lab integrations and the complexity of data formats, development costs generally range from $12,000 to $25,000.
Alerts, Notifications, and Reminders
Automated alerts and notifications keep patients and staff informed about upcoming appointments, medications, test results, and follow-ups. This module involves backend logic for triggers, scheduling notifications, and integrating SMS/email services. Development of a robust alert system typically costs $4,000 to $9,000, depending on the frequency, personalization, and channels used.
Analytics and Performance Dashboards
Analytics dashboards provide operational insights, patient flow metrics, revenue tracking, and clinical performance indicators. Developing this module involves designing data pipelines, visualization dashboards, and report generation tools. Advanced analytics, predictive insights, and interactive dashboards increase cost and complexity. The estimated development cost for analytics modules is $10,000 to $35,000, depending on data volume and reporting sophistication.
Security and Role-Based Access
Security is critical in patient management systems. This module includes role-based access control, encryption, audit logs, multi-factor authentication, and compliance with standards like HIPAA. Implementing security requires both backend and frontend development and regular testing for vulnerabilities. Development costs for the security and access control module typically range from $6,000 to $14,000.
Future Trends in Patient Management Software
The healthcare industry is rapidly evolving, and patient management software is no exception. Modern solutions are no longer limited to digital record-keeping and appointment scheduling; they are becoming intelligent, predictive, and highly patient-centric. By leveraging emerging technologies, healthcare providers can improve operational efficiency, enhance patient experience, and make data-driven decisions. Below is a detailed look at the key future trends shaping patient management software.
1) Artificial Intelligence and Machine Learning
Artificial Intelligence (AI) is transforming patient management software by introducing predictive and automated capabilities. AI algorithms can analyze patient histories, treatment outcomes, and diagnostic results to assist clinicians in decision-making. For example, predictive models can flag patients at high risk for chronic illnesses, readmission, or complications, allowing timely interventions.
Machine learning also enables intelligent scheduling, optimizing appointment slots based on patient history, clinician availability, and predicted no-show probabilities. These AI-driven features not only improve efficiency but also reduce costs and enhance patient outcomes.
2) Predictive Analytics and Data-Driven Insights
The integration of predictive analytics into patient management software enables healthcare providers to anticipate trends and make proactive decisions. Analytics dashboards can track patient flow, treatment effectiveness, and operational bottlenecks. For instance, historical data can help predict peak appointment times, medication adherence rates, or lab test demand.
These insights help administrators optimize staff allocation, reduce wait times, and improve patient satisfaction. Predictive analytics also supports population health management by identifying high-risk groups and planning preventive care strategies.
3) Telemedicine and Remote Patient Monitoring
Telemedicine has emerged as a critical component of modern healthcare, especially following the global push for remote care solutions. Patient management software now often integrates video consultations, chat systems, and remote monitoring tools.
Wearable devices and IoT sensors can send real-time health data—such as heart rate, glucose levels, or blood pressure—directly into the patient record. Clinicians can then review trends, detect anomalies, and provide guidance without requiring in-person visits. This trend not only expands healthcare access but also reduces hospital readmissions and enhances chronic disease management.
4) Cloud Computing and Scalability
Cloud-based solutions are becoming the norm for patient management software, offering flexibility, cost-effectiveness, and scalability. Cloud infrastructure allows healthcare providers to securely store vast amounts of patient data while ensuring real-time access from multiple locations.
Cloud computing also enables seamless integration with third-party services such as laboratory systems, pharmacies, insurance providers, and telemedicine platforms. Additionally, cloud-based systems simplify software updates, backups, and disaster recovery, ensuring that patient data remains secure and accessible at all times.
5) Mobile Health (mHealth) and Patient Engagement
Mobile health applications are increasingly integrated into patient management software to enhance patient engagement. Patients can now book appointments, access medical records, receive notifications, and communicate with their providers via smartphones.
Mobile apps also facilitate medication reminders, teleconsultations, and digital health tracking. High patient engagement leads to improved adherence to treatment plans, better outcomes, and higher satisfaction rates. Developers are focusing on creating intuitive, accessible, and secure mobile interfaces to maximize adoption.
6) Integration with Wearables and IoT Devices
The growing prevalence of wearables and IoT devices provides an opportunity for continuous health monitoring. Patient management software can now collect data from smartwatches, glucose monitors, blood pressure devices, and other sensors.
This real-time data is invaluable for chronic disease management, early intervention, and personalized treatment plans. Integration with these devices allows clinicians to detect issues early, reduce hospitalizations, and deliver more precise care.
7) Automation of Administrative Workflows
Automation is increasingly being applied to administrative tasks within patient management software. Features such as automated appointment reminders, billing, insurance claim submission, report generation, and follow-up scheduling reduce manual effort and errors. This not only improves operational efficiency but also frees up staff to focus on patient care.
Automation also enables consistent compliance with healthcare regulations, minimizing the risk of human error in critical processes.
8) Enhanced Security and Compliance
With the increasing digitization of patient data, security and regulatory compliance continue to be key trends. Future patient management software will incorporate advanced encryption, multi-factor authentication, and blockchain-based data integrity solutions.
These measures ensure that sensitive patient information remains secure and tamper-proof. Compliance with regulations such as HIPAA, GDPR, and local healthcare standards will continue to drive software architecture and security design.
9) Interoperability and Standardized Data Exchange
Interoperability is becoming increasingly important as healthcare providers adopt multiple digital systems. Patient management software is evolving to support standardized data formats like HL7 and FHIR, enabling seamless data exchange between hospitals, labs, pharmacies, and insurance networks. Interoperable systems enhance care coordination, reduce redundant tests, and ensure that clinicians have complete and accurate patient information at every point of care.
10) Artificial Intelligence-Powered Chatbots and Virtual Assistants
AI-powered chatbots and virtual assistants are increasingly being integrated into patient management systems. These tools can handle routine patient queries, guide patients through appointment bookings, provide medication reminders, and even offer preliminary symptom assessments. By automating routine interactions, chatbots reduce the workload on staff, enhance patient satisfaction, and ensure timely responses to inquiries.
Sum up
Building a comprehensive patient management software system is no longer a luxury but a necessity for modern healthcare providers. Such systems streamline hospital workflows, improve patient care, and optimize administrative operations.
From patient registration to appointment scheduling, digital health record management, billing, telemedicine, and analytics, every module plays a crucial role in creating a seamless healthcare experience. The software not only reduces manual paperwork but also enhances accuracy, ensures regulatory compliance, and improves overall efficiency across departments.
Investing in patient management software development allows healthcare providers to centralize and secure patient data, reduce human errors, and improve communication between staff, patients, and external stakeholders such as laboratories and insurance companies.
The integration of telemedicine, mobile apps, and patient portals empowers patients to take an active role in their healthcare, improving engagement and adherence to treatment plans. Furthermore, advanced modules like lab integrations, alerts, analytics, and AI-driven insights enhance decision-making, operational efficiency, and long-term planning.
Looking to the future, patient management software is poised to become even more intelligent, predictive, and patient-centered. With trends like artificial intelligence, machine learning, predictive analytics, telemedicine, cloud computing, mobile health, IoT integration, and automated workflows, healthcare organizations can deliver more precise, proactive, and personalized care.
Enhanced interoperability and robust security measures ensure that patient data is accessible yet protected, supporting both clinical excellence and regulatory compliance.
In essence, patient management software development is a strategic investment that transforms healthcare operations, enabling providers to deliver higher-quality care efficiently, safely, and cost-effectively.
By adopting modern technologies, healthcare organizations not only meet current operational demands but also position themselves to adapt to future healthcare trends, ultimately benefiting patients, staff, and the broader healthcare ecosystem.
FAQs
What is patient management software development, and why is it important?
Patient management software development refers to the process of creating digital systems that help healthcare providers manage patient information, appointments, medical records, billing, and communication efficiently.
It is important because it reduces manual paperwork, minimizes errors, improves workflow efficiency, ensures regulatory compliance, and enhances patient satisfaction. Well-designed software allows clinicians and administrators to access accurate, real-time data, enabling faster and more informed decision-making.
What are the key features included in patient management software development?
Patient management software typically includes modules for patient registration, digital health records, appointment scheduling, billing and insurance processing, e-prescriptions, lab integrations, telemedicine, patient portals, notifications, analytics, and security features.
These features work together to streamline operations, improve communication between staff and patients, and provide actionable insights through analytics dashboards. Advanced systems may also include AI-powered predictive tools, mobile access, and integration with wearable devices.
How does patient management software development differ from hospital management software development?
While both systems aim to improve healthcare operations, hospital management software development is generally broader and may cover additional hospital-wide administrative functions such as inventory management, human resources, staff scheduling, facility management, and pharmacy management.
Patient management software development, on the other hand, focuses primarily on patient-centric workflows, including record keeping, appointments, treatment tracking, telemedicine, and billing. In many cases, patient management modules are integrated within larger hospital management systems.
What factors influence the cost of patient management software development?
The cost is influenced by multiple factors including the number and complexity of features, third-party integrations (like labs, pharmacies, and insurance), compliance with regulations such as HIPAA or GDPR, security requirements, development region, platform choice (web, mobile, or both), and ongoing maintenance needs.
Typically, a full-featured patient management system costs between $80,000 and $250,000+, with annual maintenance accounting for 15–25% of the initial investment.
How is patient management software improving patient care and operational efficiency?
By centralizing patient information and automating administrative tasks, patient management software reduces errors, prevents duplicate tests, and ensures that clinicians have real-time access to complete medical histories.
Automated reminders, telemedicine, and patient portals enhance engagement and adherence to treatment plans. Analytics dashboards provide insights into operational efficiency, patient flow, and financial performance, enabling better resource allocation and decision-making.
Ultimately, the software improves both patient care quality and hospital efficiency while reducing operational costs.



